Two years ago, Austin Chillman didn’t spend most of his day in bed exhausted and in pain. Back then Austin was a hearty 12 year old with a slew of friends and little time to spare. When he wasn’t in school Austin threw himself into his sports –especially hockey, camping, fishing, hunting or working the trapline with his grandfather. But in August 2014, Austin’s carefree adolescent lifestyle took an abrupt turn.
When Austin wasn’t in bondage to the bathroom for up to 40 minutes a stretch, multiple times a day, he was in bed -as white as his sheets, eyes ringed with black circles, arms wrapped around his aching stomach. Everyday tasks like going to school became an unbearable endurance that often resulted in phone calls to his mom to collect him from school so he could suffer fatigue, bouts in the bathroom and pain in the privacy of his home. Even what Austin loved came with consequences. Once he could play all day long but now Austin could only last about 30 minutes in a road hockey game with friends before he returned to the couch with an aching stomach and a blood drained face.
Life spiraled out of control quickly for Austin. Physically unable to attend classes, Austin was set up for home schooling and his beloved game for hockey was benched. As Austin’s physical world began to shrink, so did the size of his social network. His loving family was bewildered, seeking answers from the medical community and finding none.
*****
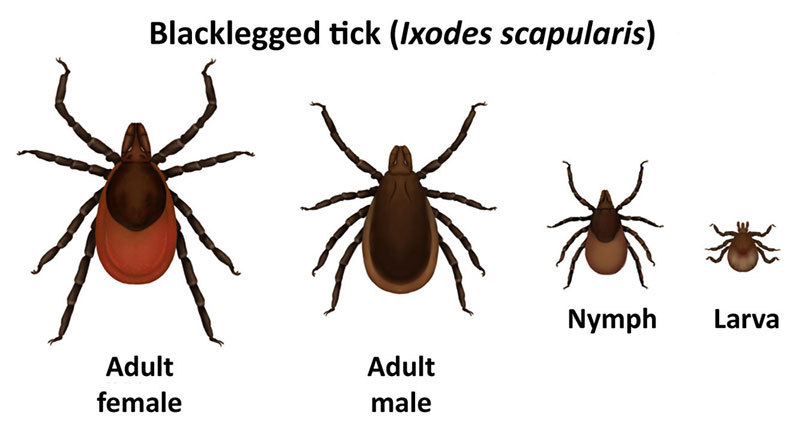 CanLyme defines Lyme as a “borreliosis caused by borrelia bacteria, which commonly infects woodland animals like mice or deer. Ticks pick up the bacteria by biting infected animals, and then pass it on to their human hosts. The are many strains or genospecies of borrelia that cause Lyme disease (borreliosis) in humans just as there are many strains of the flu virus that cause flu symptoms in humans, with some strains more virulent than others.”
CanLyme defines Lyme as a “borreliosis caused by borrelia bacteria, which commonly infects woodland animals like mice or deer. Ticks pick up the bacteria by biting infected animals, and then pass it on to their human hosts. The are many strains or genospecies of borrelia that cause Lyme disease (borreliosis) in humans just as there are many strains of the flu virus that cause flu symptoms in humans, with some strains more virulent than others.”
Despite the existence of multiple strains of the borrelia bacteria that causes Lyme, Canada only tests for one strain rendering startling inaccuracies in testing. In an interview with CBC Debra Fraleigh, co-founder of the Ontario Lyme Alliance stated that only 33 to 49% of early-stage tests are accurate due to not testing for multiple strains. An additional challenge in diagnosing for Lyme is the widespread acceptance that individuals exposed to Lyme will present a bulls-eye rash. However, CanLyme reports that only 9% of people infected by borrelia will display the tell-tale rash.
As a result of inefficient testing in Ontario, Lyme disease is often misdiagnosed and under-diagnosed. Lyme disease has been referred to as ‘the great imitator’, it’s symptoms and co-infections often confused for other diseases like lupus, arthritis, multiple-sclerosis, fibromyalgia and even brain conditions like Alzheimer’s, mood disorders and dementia.
To date, public health policy in Ontario does not accept what some research shows to be that Lyme disease can be a chronic condition. Currently, early interventions are touted as the cure for Lyme disease but data has demonstrated that Lyme can recur in patients despite early treatment with aggressive rounds of antibiotics.
Further, research on borrelia and Lyme that has been accepted by the United States and some European countries has yet to be incorporated into the development of a provincial public health strategy in Ontario. In fact, the Association of Medical Microbiology and Infectious Disease Canada and Public Health Ontario –the entities that shape public health policy in Canada, question the research that has been informing Lyme policy development in other countries for years.
The challenge in diagnosis and treatment for Lyme in the province has driven many Ontarians into the United States –and often into debt, to seek answers and help for their ailing health conditions. Doctors in Ontario who have dared to progressively diagnose and treat Lyme in their patients have been harassed by peers and some have lost their license to practice. Other doctors have packed up and moved their practices to British Columbia or into the United States where the medical as well as naturopathic interventions for Lyme are far more enlightened and effective. ‘Rogue’ doctors who remain in Ontario and treat their patients for Lyme –outside of the sanctioned guidelines of Public Health Ontario and the College of Physicians and Surgeons of Ontario, do so under the radar, encouraging their patients to not speak of the treatment that they are receiving.
The lack of an efficient public health policy in Ontario that will diagnosis for all strains of borrelia has been highly criticized by Manitoulin-Algoma Member of Provincial Parliament, Michael Mantha whose Private Members Bill to develop an action plan on Lyme disease received unanimous passage in November of 2014. There is much work to be done.
“There’s a lot of people affected by Lyme disease across the province –it’s not just in Southern Ontario. This is a chronic disease that is growing at ridiculous paces. We need to make sure our healthcare professionals are prepared and literate about Lyme and how to react to Lyme disease,” stated Mantha. “Very bluntly, the problem here is Public Health Ontario. They are failing to recognize the work and the treatments that have been done across the U.S. and other countries. We need to bring those health professionals to Ontario and hear what they have to say. Unless we get our doctors educated about Lyme –so that people are tested and treated for it, we’re going to continue to spend millions of dollars to treat people for diseases that they do not have instead of treating them for Lyme.”
The Ontario Lyme Disease Clinic reports that, “In the United States and Europe, where much of the research is being conducted, researchers consider Lyme a larger pandemic than Cancer and AIDS with estimates of up to 200,000 new cases a year in the United States.”
*****
When the bad stomach episodes began in the summer of 2014, Austin’s mom, Vicki Chillman, chalked it up to a touchy stomach. Austin was a sensitive kid, explained Vicki, who had a tendency to think too much, worry about people and sometimes internalize his feelings. The year leading up to Austin’s sudden illness was a difficult one for the entire family. The family lost their dearly loved dog and lost three family members to cancer –including an aunt that Austin was very close to. That fall Austin was also moving to a new school.
Vicki decided to keep an eye on what Austin was eating, keeping a food journal and documenting when Austin would have flair ups with his stomach. Wheat seemed to be troublesome and when eliminated from Austin’s diet he showed improvements, requiring less time in the bathroom but still left with a ‘stabbing pain’ at the top of his stomach.
Unsure if the switch to the new school was creating possible anxiety for Austin, Vicki even pursued counselling for her son. “I put him in counselling because I thought he was getting bullied. The counsellor said that Austin was really well-rounded and easy going. I even had a ‘spy’ at school who said that she didn’t see anything going on and that Austin had lots of friends,” recalled Vicki.
After ruling out issues at school, and when Austin’s pain and fatigue persisted after diet modifications, Vicki and her husband pursued the expertise of the medical community. So would begin nearly two years of myriad testing and diagnosis. And for Austin and his parents, the worst of it all was the belief from many Canadian health professionals -and even trusted friends and family, that the origin of his physical illness was in his head.
“Our doctor here thought it was psychosomatic. He thought it was a psychological problem or an eating disorder. He said Austin was using food as a control,” remarked Vicki. “Austin loves to eat, he wants to eat.”
Austin’s unexplained symptoms were increasing, the most severe of them included: chills; fatigue; shortness of breath; stomach upset; change in bowel function; daily headaches; neck pain; poor short-term memory; disorientation; joint pain; and a disturbed sleep pattern.
*****
Jim Wilson, president of CanLyme, also lives with a diagnosis of Lyme disease. “The government has been misleading Canadians for a long time about the accuracy of testing. Current testing for Lyme disease has shown that the reliability is in fact worse than the toss of a coin.”
The earliest case of Lyme’s was traced back over 5,000 years ago when an ice mummy was discovered in the Eastern Alps. Genetic testing indicated the presence of Lyme in the joints of the mummy. The revelation indicates an unpleasant symbiotic relationship between man and borrelia that has thrived for centuries. Wilson criticizes Canadian research that focuses on the study of ticks. “We have a serious problem. And we have science and technology at our disposal yet we are doing nothing. We’re still studying ticks. We’ve got thousands of sick Canadians that we need to be studying.”
More so, Wilson asserts that Lyme patients and their experts must be included in the development of a new Lyme public health strategy in Canada. He is hopeful that the with the unanimous support for Bill C-442 in the House of Commons a year and a half ago that that is exactly what will happen. The Bill establishes “a framework for collaboration between the federal, provincial and territorial Health Ministers, representatives of the medical community, and patients’ groups to promote greater awareness and prevention of Lyme disease, to address the challenges of timely diagnosis and treatment, and to push for further research.”
“If this unfolds as it should,” remarked Wilson, “we are going to proceed as equal partners with the intention of seeing a complete change in the direction of research in Canada. And the public has to start demanding that. We are currently spending a ton of money managing this huge single user group of the healthcare system- the chronically ill. The chronically ill are the largest users of our system. We have two million chronically ill people with labels like chronic fatigue, fibromyalgia, lupus, irritable bowel syndrome and psychiatric disorders. We know a percentage of those are misdiagnosed and those patients are very apt to have Lyme disease. We just don’t know what the percentage is but we believe it to be very significant. There’s certainly a lot of money made managing symptoms as opposed to curing the disease.”
*****
Having grown frustrated with the lack of a diagnosis for Austin, Vicki plead with the family doctor for a referral to The Hospital for Sick Children in Toronto. The physician complied with the request but only with the accompanying condition that Austin would speak with an adolescent medicine mental health doctor while there. With nothing to lose, Vicki agreed and so the family headed to SickKids in April 2015. After only a 15 minute interview with Austin, a mental health doctor agreed with the family doctor’s diagnosis that Austin’s pain was psychosomatic. However, one of the three doctors that met with Austin was amenable to ordering up a couple of scopes for him. An endoscopy and a colonoscopy were scheduled for November 2015.
Over the 7 months between visits to SickKids, Vicki pursued other options in the hopes of making her son well. Through the grapevine Vicki heard about the Born Clinic in Grand Rapids, Michigan. She called the facility and the clinic was able to schedule her an appointment immediately. In May 2015, Vicki packed up Austin and headed to the clinic where he underwent a battery of bloodwork and surrendered stool and hair follicle samples. Within a couple of weeks the results of the work up showed that Austin had an overgrowth of yeast- candida, food insensitivities, an amazing vitamin D deficiency and an astonishing high level of cadmium- a heavy metal, in his body. The findings were affirming but left Austin’s parents with questions like ‘why does our kid have high heavy metal?’ and ‘why does our kid have candida?’ and ‘why does our son have really low Vitamin D?’ and ‘why does he have chronic fatigue?’.
“We had to eliminate a bunch of food and then reintroduce them into his diet. He wasn’t deathly allergic to anything but food was playing games with him. And he had yeast everywhere,” remarked Vicki.
Austin was loaded up with vitamins and supplements and a prescription was issued to help him fight off the overgrowth of yeast in his body. Things got better for a while.
“We got our kid our kid back last summer. I’d ask Austin about his pain level and some days it was a 5 out of 10 – we hadn’t gotten a 5 in a long time. But he still had pain. He shouldn’t have had any pain- he’s a kid. But we’d go to the mouth of the river and we’d go swimming and then he’d come home and the next day he would be pooched. If he did a lot in a day, the next day he always paid for it. He was cautious to do anything too much. He knew he would be in more pain,” remarked Vicki.
Waving a list of all the foods Austin needed to avoid Vicki added, “And the diet was ridiculous. Thank God we have hunters in the family. We feed him wild meat. And I have to make gluten free bread- and no sugar because he has candida and sugar feeds candida.”
The summer of 2015 ended and so did Austin’s prescription for candida. Austin went back to school, maybe things would return to normal. But by the end of September Austin’s health began to backslide. This time the pain was far more exquisite but to add to his suffering, as well as his parents, was the ever growing criticisms from doctor’s and acquaintances. Unhelpful comments came from every direction – “just make him go to school” and “he’ll get over it” and “there’s nothing physically wrong with him” and “it’s a psychological condition” and “don’t you think your son is playing you a bit” and “if that was my kid”.
Vicki believes her son experiences pain on a daily basis. She does not believe, however, that his physical pain is a symptom of a mental health issue. Vicki also believes that the chronic pain Austin experiences, as well as the suspicion from health professionals and acquaintances that he is contriving a physical illness, does put Austin at risk to acquire a mental health injury like anxiety or depression.
*****
For many people who suffer from Lyme’s disease- diagnosed, misdiagnosed or undiagnosed, mental well-being can be impacted by the perceptions of the medical community and loved ones who don’t believe the individual is physically suffering. Add to that the very real presence of chronic pain and the risk to suicide can increase.
The Canadian Mental Health Association reports that among people with chronic pain, the prevalence of flourishing mental health declined as pain intensity and the number of activities prevented by pain increased. According to data from the U.S. National Comorbidity Survey, compared with the general population, individuals with chronic pain have a significantly higher prevalence of depression (20.2% vs 9.3%), posttraumatic stress disorder (10.7% vs 3.3%), and any anxiety disorder (35.1% vs 18.1%). Research conducted by the Department of Psychology, Institute of Psychiatry at King’s College in the United Kingdom concluded that patients with chronic pain are twice as likely to commit suicide compared to patients that did not experience chronic pain.
Studies suggest that the development of suicidal ideation among people who experience chronic pain “arises from the confluence of two factors: thwarted belongingness –unfulfilled need for social interaction or connectedness; and perceived burdensomeness –perceiving oneself as a burden or liability to others.
To further exacerbate the risk of suicide among people with Lyme, the multisystemic illness can affect psychiatric issues like depression and anxiety.
“The loss of life among people with Lyme is happening coast to coast. Sometimes it’s a death that has occurred because an attack on the person’s organs and sometimes people are committing suicide,” remarked Wilson. “There’s two very distinct forms of depression that comes with Lyme. There is the actual psychiatric disorders that can be caused by the borrelia bacteria playing havoc in the brain and then there is the depression that comes from just being sick -and being looked at with disdain by the medical community. You are not listened to. You’re often marginalized within the system –in fact almost always if it’s anything to do with Lyme disease. So that causes a sense of hopelessness and fear and that brings mental health issues.”
*****
That November the second visit to SickKids for Austin’s scopes rolled around. The good news was there wasn’t any sign of bowel disease but tests did indicate that the top of his stomach was inflamed. So it was another trial and error of taking away and then re-entering supplements into Austin’s daily regime and keeping a strict and challenging diet- both for Austin and the chef, his mother.
Concerned for her mental well-being, Vicki’s husband begged her to leave her full-time job. The nature of his employment required him to be away from home for periods of time leaving Vicki to care for not only an unwell son with very specific, and at times very demanding needs, but also a young daughter. Added to that were the needs of a close family member who became gravely ill and relied on Vicki during his recovery. Now home as a round the clock caregiver, Vicki also became a full-time researcher.
“I thought, well, if I’m going to be home every day I’m going to throw myself into this. I’m planning meals and I’m researching. I’m going to get him better,” commented Vicki. “So I researched Austin’s symptoms and Lyme disease kept popping up. So I called the Born Clinic again and they sent me the Lyme’s checklist. They told me to fill it out and the results of the checklist would tell us if we needed to do testing for Lyme.”
Through her research Vicki discovered that Canada had a dismal track record for the diagnosis and treatment of Lyme disease. She knew if she wanted Austin to be thoroughly tested for Lyme her best bet was to take him back into the United States
“I had researched enough to know that most Canadian testing for Lyme comes back negative because they only test for one strain of Lyme. It’s ridiculous,” stated Vicki. The family hopped across the ditch to the Sault Memorial hospital in Sault Ste. Marie Michigan. Blood was drawn but Vicki would learn after that the samples were sent to a lab that didn’t thoroughly test for Lyme.
Speaking with new found Lyme mentors online Vicki discovered that the most innovative testing for Lyme was being conducted at IGeneX – a lab in Palo Alto, California. So –back to the Born Clinic for bloodwork that would be sent to IGeneX. In February 2016, finally, the results came back showing neither a positive result nor a negative result for Lyme. Findings from Austin’s bloodwork showed that he tested positive for 2 of 5 strains of Lyme yielding an indeterminate result –a common finding among Lyme sufferers.
The discovery of Lyme disease in Austin’s system and an indeterminate diagnosis was a catch-22. Vicki found herself sitting at the kitchen table once again, playing doctor. What should she do? Set her son up with an aggressive series of antibiotics to treat Lyme disease that could also have horrifying side effects? Or should she pursue even more testing?
*****
The experts are divide on the matter of reliable testing for the presence of Lyme disease. The Ontario Lyme Disease Clinic indicates that two tests have been approved in Canada (keeping in mind that Canada does not test for all strains of Lyme) and the U.S. – the ELISA and the Western Blot. However, both tests are recognized to have limitations including up to 50% in false-negative results. The debacle of diagnosing reinforces the need for improved testing and the urgency for a provincial and federal public health strategy for Lyme disease.
To mitigate the boundaries of testing, doctors have begun diagnosing patients not just based on testing but also symptomatology. Also, the success of clinical treatment trails can affirm a diagnosis of Lyme disease in a patient.
“Quite often it is the treatment that substantiates the diagnosis,” remarked Wilson. “Most people have been floundering in our medical system for quite some time before they get to that point, with no improvement whatsoever, and often horrible side effects from being put on medication that they don’t need. Once they get the proper diagnosis and go on treatment, it’s only then that they start getting their health back. And that supports the diagnosis.”
In 2009, British Columbia was the first, and remains the only, province that has sanctioned naturopaths, who have successfully completed provincial pharmacology exams, to order tests and prescribe medication- such as antibiotics, to treat Lyme. The Born Clinic in Grand Rapids –the clinic that Vicki brings Austin to, combines conventional medical interventions with naturopathic interventions, creating a holistic treatment process.
*****
Today, aside from a supportive nurse practitioner at the Group Health Centre, Vicki has given up on the local medical community. “We don’t bring Austin to our doctor anymore or even the emergency at the Sault hospital. When I take him there they just tell us to go home and that there is nothing wrong with him. You’re on your own. The only people that can help you are people that are similar to you. That was the hardest part- I’m alone, I have nobody.”
To manage his symptoms Austin is taking on a daily basis, 3 multivitamins, 2 supplements for yeast control, 2 probiotics, liquid aloe and liquid silver. Austin is also set to begin taking amitriptyline -a nerve prescription, in the hopes that it will lessen his newly acquired leg pain that keeps him bed ridden at times.
“For the last three months he’s had extreme pain in his legs. He has these little balls in his legs- they’re like cysts. There are days that he can’t walk down our stairs because his legs are so sore,” shared Vicki.
Vicki’s family are not unlike many Canadians who have gone abroad and into debt to seek answers and treatment for a loved one’s ailing health. Travel grants only apply for those who receive treatment in Canada- and that reimbursement has been woefully inadequate for years. The family, with a bit of support from Vicki’s parents, have sunk about $40,000 into travel, testing, medication and treatment for Austin. Add to that debt the loss of Vicki’s full-time income to care for her son –and family, as well as to preserve her own sanity through the mind-bending mystery of the medical system and her son’s illness.
“It used to bother me that we don’t have siding on the house- I don’t care anymore,” admitted Vicki. “I don’t care that we have to go without certain things because I’m not working. It doesn’t matter. I just want Austin to be better.”
Recently, a benefit was held in Thessalon –the small community where the family lives, about 50 minutes east of Sault Ste. Marie, Ontario. The family is grateful for the generous donations that were raised by the town and close family and friends.
Over the short-term Vicki has decided to maintain the regular course of pain management and symptom control for Austin. Today she tells people that Austin is being treated for Lyme disease. Vicki is understandably acrimonious and tearful when she says, “Having a name for what Austin is experiencing makes people more sympathetic. That bothers me a bit. All we have hoped for from other people is that they would be compassionate and not judge. But people judge hard core. I feel bad for anyone who has chronic pain or illness because people don’t get it. People say it’s all in their head.”
In July 2016 Austin will be travelling to Whitby, Ontario to meet a Lyme literate doctor. Vicki hopes that the outcome from this visit will remove the burden of diagnosis from her shoulders when a doctor finally says ‘yes, Austin’s bloodwork for Lyme is indeterminate’ and ‘yes, Austin’s Lyme’s checklist is concerning’ and ‘yes, Austin has Lyme disease. Let’s begin treatment’.
*****
Lyme diseases has been tagged as the most political and controversial disease of our times.
“The government has been failing us and failing us badly. In fact not only have they been failing us badly on this but the medical bureaucrats have been putting up roadblocks,” stated Wilson. “People with Lyme, and the experts successfully treating Lyme, can no longer just be on the outside looking in. We need to be fully engaged as equal partners in developing a Lyme strategy framework, not only federally but more importantly provincially where the actual policy and guidelines that reach into the doctor’s office, the patient-physician relationship, treatment guidelines and surveillance and prevention, are developed.”
Mantha has drafted a petition calling for the urgent creation of an Action Plan on Lyme Disease.
“Austin’s mom and dad are beautiful loving parents who want to try to provide the best care for him and they’re realizing what many others have brought to my attention -you can’t do that with Lyme disease in Ontario,” remarked Mantha. “Austin, as an Ontario resident, is being discriminated against based on his illnesses. He’s being told it’s all in his head, that they’ll schedule him an appointment with a psychiatrist, to move on. Mom has also been suffering- although Austin is the one with Lyme disease, the entire family is coping with this. There is a frustration and helplessness in not being able to do anything. You look at changing diets, vitamins, your habits- you look at all other avenues and then at the end of the day it’s not working. The pain is still happening. The young boy is still suffering constantly from this. He just wants to be a boy and have fun. Why are we denying him that opportunity? He use to play hockey- that’s what he’s supposed to be doing. He’s not supposed to be fighting Lyme disease and the government.”
*****
Stepping onto a public platform hasn’t been easy for Vicki. Compelled by a fierce love for her son and convicted by the truth of their experience fighting Lyme disease and a government that denies the prevalence of it, Vicki mustered her fighting spirit and laid it all out for the world to see.
“I want people to know Lyme disease is out there –and here in Northern Ontario, in Algoma. People with Lyme disease are being misdiagnosed with lupus, fibromyalgia, chronic fatigue syndrome- all sorts of things. If anyone has symptoms all over the map and nobody can figure out what is wrong, go and get tested for Lyme in the States. And I want people to not buy in that chronic pain is just in somebody’s head. Especially if it is a kid.”
Vicki’s voice drops and her eyes mist up. “We’ve lost friends in this. But I guess they really weren’t friends. It’s hard for Austin to understand. He’s just a kid. So, when somebody is sick, please don’t forget about them. Don’t stop inviting people to do things. Keep asking even if you get a ‘no’ more than a ‘yes’. It’s just important that you’ve been asked.”
*****
To learn more about ticks, prevention, diagnosis and treatment check out CanLyme, Lyme Ontario or Ontario Lyme Alliance.
Want to send a message to the government? Contact your MPP and don’t forget to sign your name to this Lyme Disease Petition.







2 Comments
The symptoms of Lyme disease are exactly the same as the symptoms of thyroid/adrenal problems so I believe that Lyme disease may attack the Endocrine system. In fact, the 60 symptoms of Lymes disease are all thyroid related. Your endocrine system controls your immunity –if it’s not working properly your body can’t fight off disease. The symptoms this Mom described –fatigue, I.B.S, hives are consistent with the symptoms of Hypothyroid ( I have them too) and to be treated for it you need an integrative doctor or a naturopath that does full thyroid/adrenal testing and who tests/treats Lyme disease. You will not get this from mainstream medicine. They stopped recognizing and properly treating thyroid problems 40 years ago.
Sad but an accurate account of what many Lyme patients go through. I hope the Amitriptyline (Elavil) brings relief of the nerve pain. I had great success with that. Austin is fortunate to have such a trooper of a mother; a wonderful advocate who believed her son and didn’t give up. Wishing you all the best and that the treatment is effective in helping Austin get back to leading a “normal” life as quickly as possible.